A while ago, I wrote a post bemoaning the harms of unnecessary antibiotics for patients who, despite having bacteria in their urine, have no symptoms of a harmful urinary tract infection.
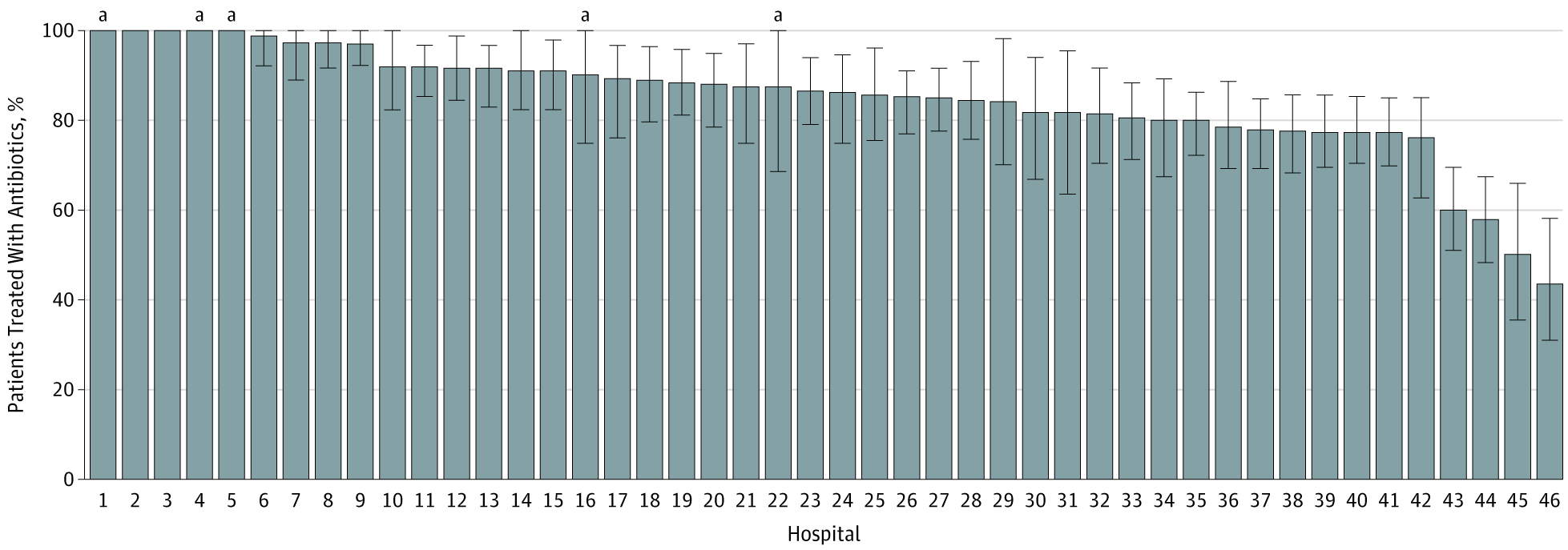
A study out of Michigan looked at how often physicians prescribe such unnecessary antibiotics, among hospitalized patients. The study discovered that antibiotic prescribing was rampant, even among asymptomatic patients.
To read the rest of this article, please visit Forbes.