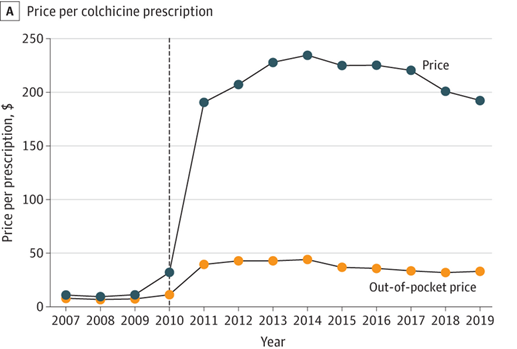
Peak Pandemic–Guess What Was Killing More Young Americans Than Covid-19
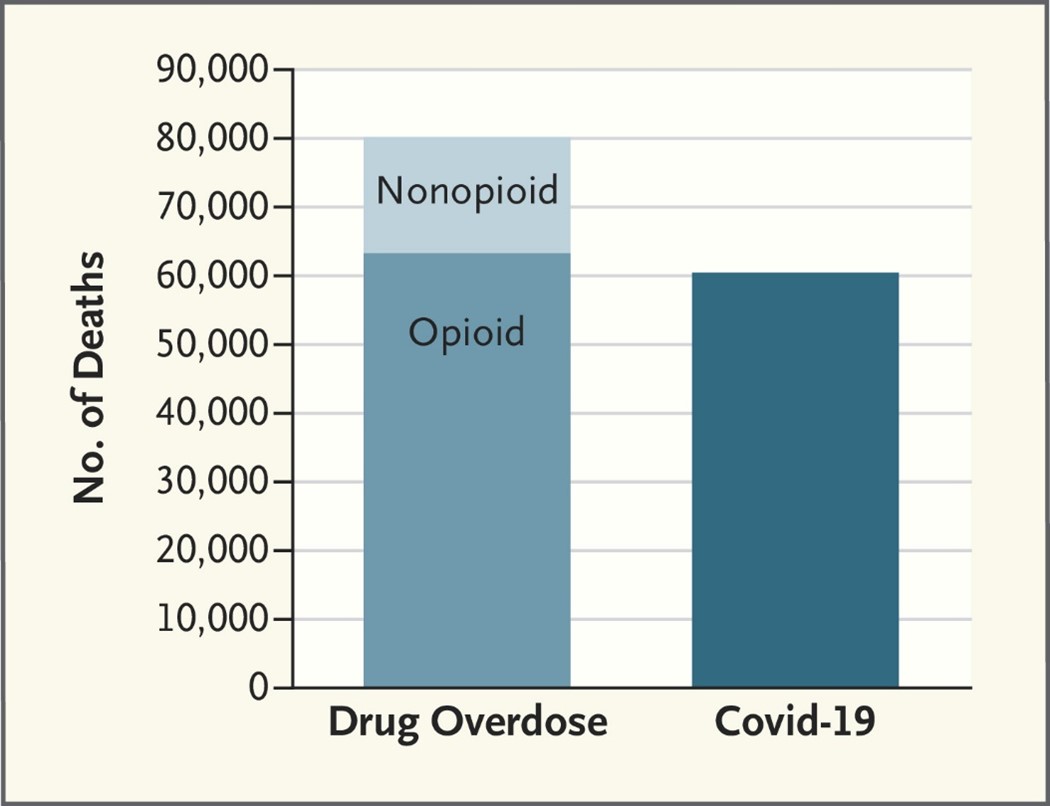
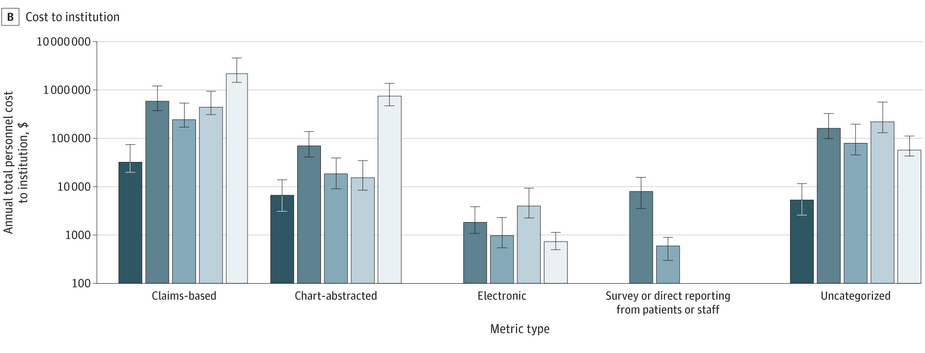
The Crushing Cost Of Tracking Healthcare Quality—One Hospital’s Story
Preventing Diabetes – What Medicare Administrators Could Learn From Shark Tank
Drugs Are Outrageously Expensive—Canada Found A Way To Fight Back
Getting What You Want At The End Of Life – Lessons From A Dying Man
Spend Too Much On Your Medications? Help Is On The Way
From Sponge-worthy to Contagion-worthy
Regulating Surprise Bills Lower Healthcare Prices – Guess How Much
Puccini Was Dying Of Cancer—Hiding His Diagnosis Was A Grave Mistake
It would have been a difficult ending under the best of circumstances. Composing what would be his last opera, Giacomo Puccini was struggling to humanize Turandot, daughter of the Emperor and a woman of mesmerizing beauty. Early in the opera, she had cruelly disposed of a series of want-to-be suitors, beheading some and torturing others, with the casual cruelty of a sociopath. In the final act of the opera, Puccini was hoping to compose a compelling, yet plausible, aria that would thaw her icy cold heart without asking the audience to forget, or even forgive, her sadistic past.
Puccini’s struggle was made all the more difficult because he was suffering from persistent pain in his throat.