For much of the history of U.S. medical care, hospitals and physicians have existed as separate financial entities. Physicians in the U.S. have typically been self-employed, as solo or group practitioners and not as hospital employees. An internist like me might have admitting privileges to several local hospitals. When we admit patients to one of those hospitals, we bill insurance for our services. The hospitals send insurers separate bills for hospital related expenses. Physicians and hospitals have depended on each other to conduct their business, but they have done so while largely maintaining their financial independence.
The U.S. government is trying to change that. The Medicare program is encouraging healthcare providers to consolidate forces into entities like accountable care organizations, in hopes that such integration will increase healthcare efficiency. These hopes exist because some of the most respected healthcare institutions in the country – places like the Kaiser Permanente system and the Mayo Clinic – have long integrated their physicians with hospitals. Indeed, some contend that this integration creates more efficient care.
Such integration could end up costing lots of us lots of money. When hospital and physician practices join forces, healthcare prices often rise.
That’s certainly the conclusion of a study published in JAMA Internal Medicine, led by Hannah Neprash out of Harvard Medical School. Neprash and colleagues explored what happened to healthcare spending when physicians and hospitals integrated. They discovered that outpatient spending rises as physicians gain market power through their hospital alliance. The spending increases are due almost entirely to price increases. Here is a picture of their findings. The main thing to note is that the taller bar, in each pair of bars, is the increase in healthcare prices while the shorter bar is the increase in utilization, following consolidation of physician practices and hospitals:
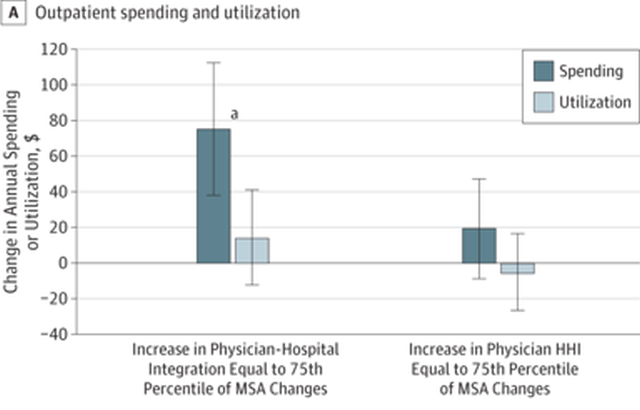
The tall bar on the left reflects a large increase in outpatient spending after hospitals and physicians integrate. The shorter bar right next to it reflects a modest, and statistically insignificant, increase in outpatient utilization at the same time. Spending rises while utilization stays flat – that can only happen because the price of services has gone up.
To read the rest of this article, please visit Forbes.
